Blog

Art and Science I: Please hold the Science
When I bring up the research from clinical psychology on outcomes of psychotherapy, other therapists say to me, “Psychotherapy is an art and a science.” Yet I’ve had one colleague say to me, “Science can’t tell us anything since it’s always changing its mind.” Another told me, “Science cannot reveal anything about therapy because therapy is about human relationships...”
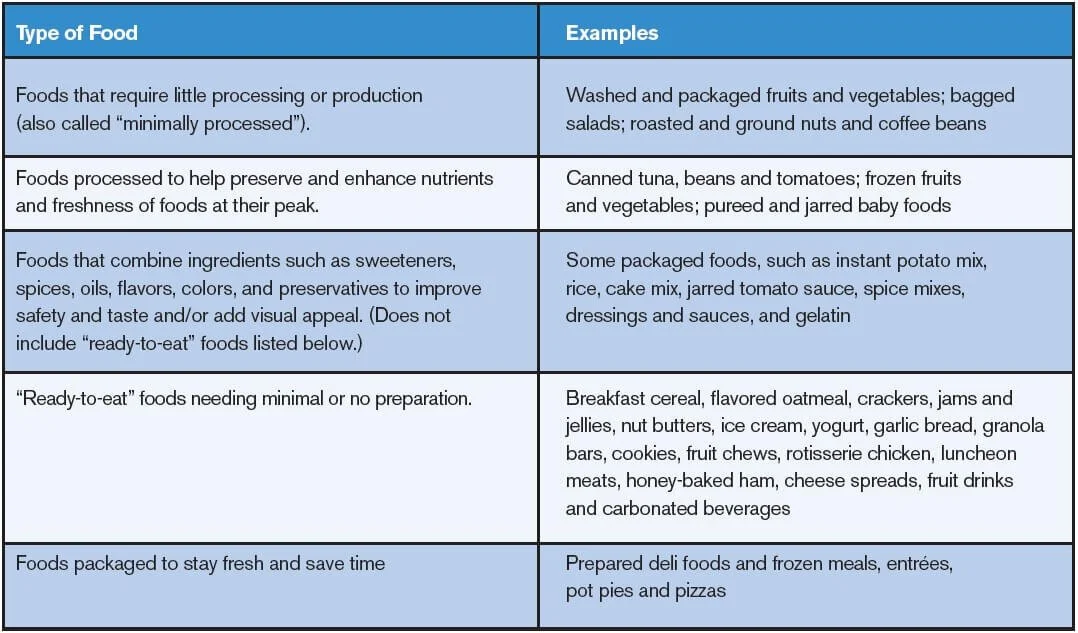
Evidence Based Wellness Choices to Make Life Better
To best understand the role of diet, exercise, and sleep, begin with a detailed journal. Using an app like MyFitnessPal is a quick way to start a food journal. Documenting is an excellent way to learn calorie and nutrition content and gain insight regarding what your choices really entail...
